Your day is full of taking payments, filing insurance claims, answering phones, scheduling appointments, and providing great dental care for your patients. With all that goes into running a successful dental organization, it’s not surprising that sometimes claims slip through the cracks and don’t get submitted.
But you don’t have to let these unsubmitted insurance claims negatively impact your cash flow. Dentrix Enterprise can help.
One important report you should be running each day is the Insurance Claims Not Sent Report. This report will identify all insurance claims that have been created in the Ledger but not sent to the Batch Processor, printed, or sent electronically through eClaims. This report is the easiest way to catch unsubmitted claims.
When you run this report, there are a variety of helpful filters. For example, you can specify a range of patients, providers, insurance carriers, and clinics to be included. You can also filter by billing type, patient tag, and by dental or medical insurance.
How to Generate the Insurance Claims Not Sent Report
- From the Office Manager, click DXOne Reports.
- Under Select Report Category, click Ledger.
- Double-click Insurance Claims Not Sent.
- Set the filters as desired and click OK.
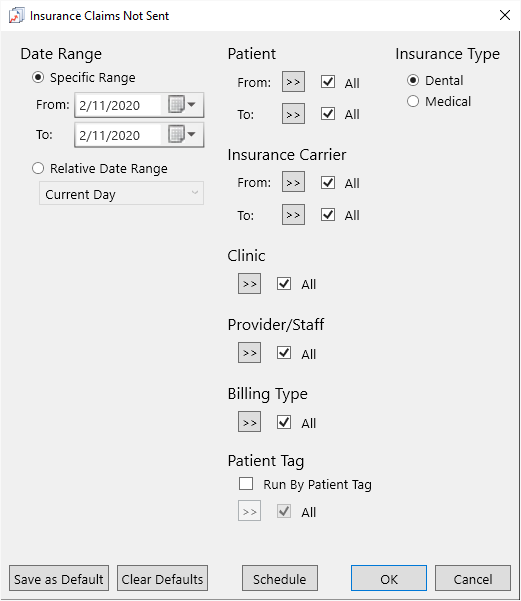
The report includes total amounts for primary and secondary claims and a combined total, to let you know just how much of your cash flow is tied up in unsubmitted insurance claims. Once you have your list of claims not sent, you can go to each patient’s ledger and process the claims.
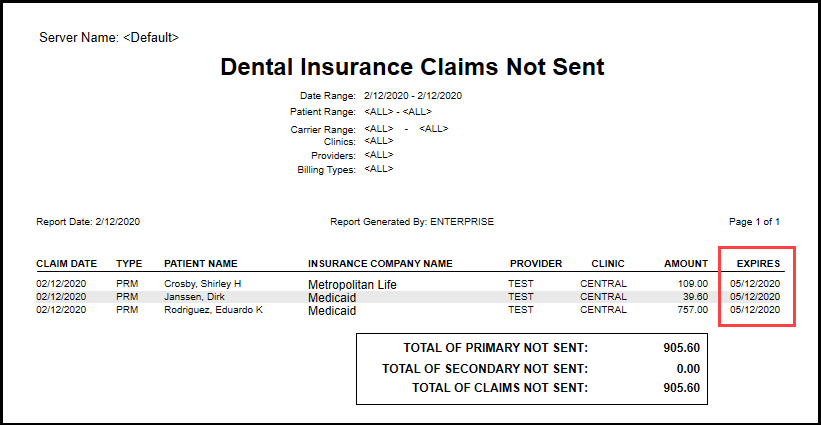
Pay special attention to the Expires column on the report. This is the deadline by which the insurance carrier must receive the claim before it expires. Make sure you process your claims before that date so you don’t negatively impact your cash flow.
Additional Information
- Deleted claims do not show up on the Insurance Claims Not Sent Report.
- To learn more about this report, view the Insurance Claims Not Sent Report section of the Reports Reference Guide.




